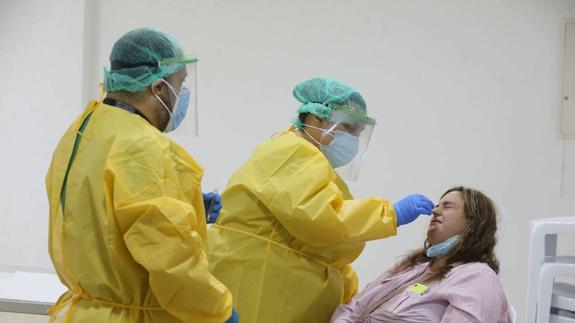
Going round in circles to get a PCR test
The battle against Covid-19 has moved to the local health centres, where doctors increasingly warn they are overstretched
ALBERTO GÓMEZ
Martes, 13 de octubre 2020, 14:48
Pressure on hospital beds in this second wave of Covid-19 is a long way off the March peak, so far. At the moment, the real healthcare battleground has switched to local public health centres, where family doctors are getting more frustrated.
Between giving advice via phone appointments and seeing people in person, these centres are now overwhelmed. On top of this is the work tracing the contacts of new Covid-positive patients, which is never ending.
To tell the authorities that you might be positive and then get a PCR test has become an ordeal of unanswered calls and waiting that tries anybody's patience.
From the moment you suspect you might have Covid-19, or symptoms appear, or somebody that you have had contact with tells you they are positive, through to getting an appointment for a PCR test, four to 12 days can go by.
As the peak viral load happens on the fifth or sixth day after getting infected, this means that by the time the average person is having a test at the moment, the bulk of their infectious stage is over.
Self-isolation dilemma
As a result, voluntary self-isolation, without an official diagnosis, becomes a difficult trade off between acting responsibly and whatever personal or work-related commitment could get in the way. All in all, these delays are helping to fan community contagion as infections go unchecked.
The average waiting time for a phone appointment in health centres is 4.6 days, according to latest regional government data. That's if you can get one, as the online app, Salud Responde, frequently advises users that there is no appointment available for 14 days.
One medic said the online systems just aren't meant for the new normal: "We are overloaded with work, we do overtime and many have put off their holidays."
Spain has fewer family doctors than the European average, 76 per 100,000 people compared to 123.
Trapped in a vicious circle
There is a fear that everyone is about to get trapped in a vicious circle, as patients who can't get phone appointments turn up in person to stand in a queue to be seen, which in turn stops doctors getting through their list of phone patients for that day. And so the cycle repeats itself the next day.
Enrique Gavilán, a doctor and also an author on health service issues, said: "We came into this crisis in such a precarious state that everything has been blown out of the water. We're now paying the price for the historic lack of investment in primary healthcare." There is a consensus that a new model is needed. "We're doctors, not administrators," he adds.
Lack of personnel to do tracing
The lack of people to carry out the tracing of contacts is also worrying the medical community. "It's a lie that they have taken on more tracers," claims one doctor asked by SUR.
The most immediate worry is the likely effects of any wave of normal winter flu, on top of the Covid-19 patients and despite masks helping stop the spread of any virus in general.
Concern over asymptomatics
One Intensive Care doctor said that the other worry is the inability to find asymptomatics. "Although they may wear a mask and respect social distancing, they do live with other people." The health authorities are therefore increasing their focus on controlling meetings in people's homes.